Uterine Cancer
What Is Uterine Cancer
Recent statistical data revealed a sharp surge in the number of uterine cancer cases reported worldwide. However, an increase is also seen in the recovery rate. According to cancer.net, 67% of cases of uterine cancer are diagnosed at an early stage which is an indication of better recovery and survival.
Unlike most cancer types, uterine cancer is more common in high-income countries. There is evolving evidence that sedentary behaviors increase the risk of uterine cancer which is a pattern seen in developed countries.
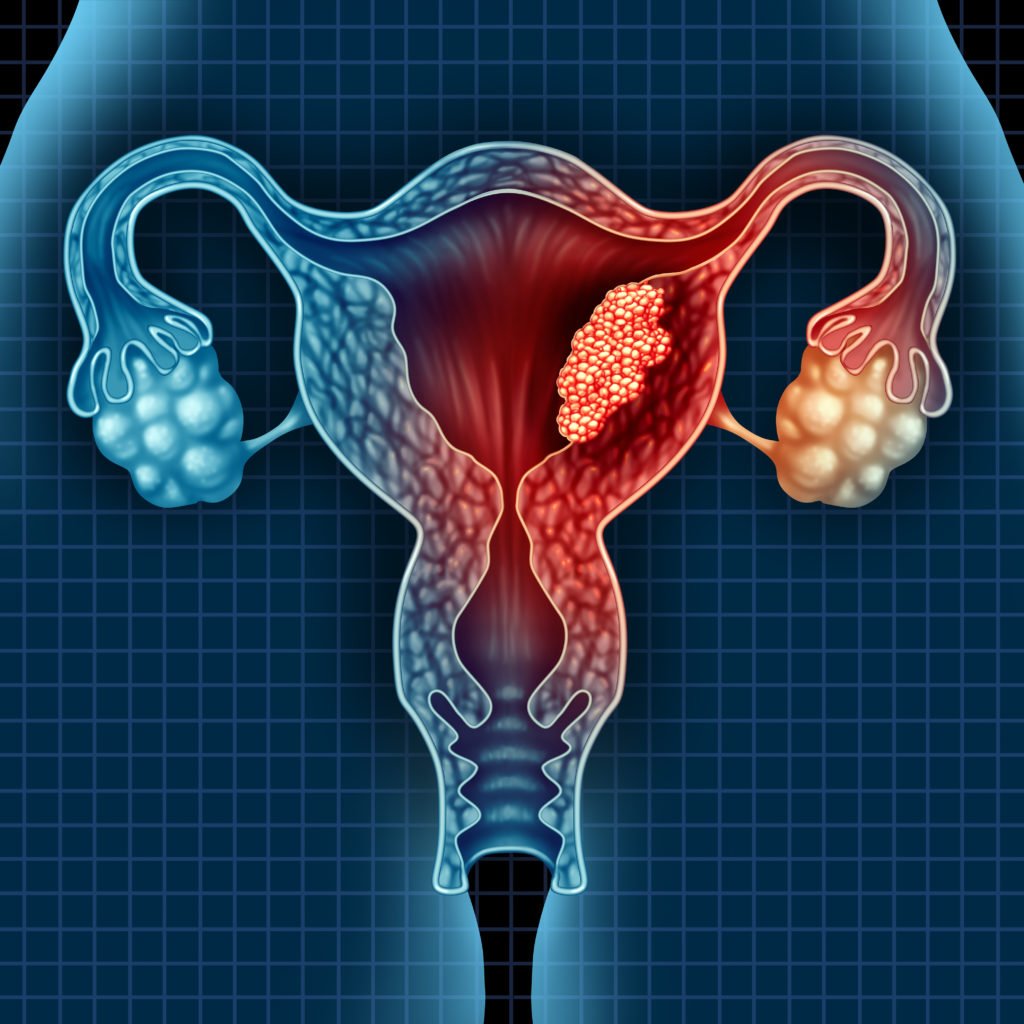
- Endometrial cancer
- Uterine sarcoma
Uterine sarcoma is the rare and aggressive form of uterine cancer that originates in the muscles or support tissues of the uterus. Uterine sarcoma accounts for 2% to 4% of all uterine cancer cases.
The uterus has two layers –
- the myometrium or the outer muscular layer,
- the endometrium, the inner lining.
- the serosa, the outer smooth layer
Anatomy Of Adrenal Cancer

Functions of the uterus
- Receiving the embryo.
- Sheltering the foetus during pregnancy.
- Delivering the newborn at term.
- Development of the embryo and foetus during pregnancy.
- Uterus also plays a vital role in the continuity of life.
Occurrence rate of uterine cancer
Uterine cancer is the most commonly diagnosed gynaecologic malignancy and it is the sixth most common cancer affecting women worldwide. Recent data on uterine cancer suggests that there has been a constant surge in the incidence rates of uterine cancer. Some of the underlying reasons for this might be –
- Early menarche.
- Stress that affects hormones.
- Increasing trends of infertility.
- Increased life expectancy of women.
- Obesity on the rise.
- A surge in the cases of diabetes.
Increased use of tamoxifen due to a surge in breast cancer cases
What Are The General Symptoms Of Uterine Cancer?
- Abnormal vaginal bleeding
- Vaginal discharge.
- Pelvic pain
- Constipation
- Pain, pressure or cramps in the lower abdomen
- Problems during pregnancy, premature contractions and spontaneous abortion.
The most common symptom of uterine cancer is abnormal vaginal bleeding. This can be bleeding between periods, bleeding after menopause, or bleeding heavier than usual. It usually starts as light bleeding with watery discharge which tends to get heavier with time.
9 out of 10 uterine cancer patients report this symptom. However, abnormal vaginal bleeding may also occur due to other issues. It is best to consult a gynecologist before reaching any conclusion.
What Are The General Causes Of Uterine Cancer?
The exact causes of uterine cancer are not yet known. However, through years of observation, study and research, a few factors have been revealed that play a crucial role in increasing the risk of cancer in the uterus.
Some of the risk factors leading to uterine cancer are controllable, like the use of hormone regulating medicines, obesity and diabetes. But most of the factors contributing to uterine cancer are beyond one’s control. Infertility, early menarche, ageing, hereditary risks are some of the natural causatives.
Ageing
The risk of uterine cancer increases with aging. Most cases of uterine cancer occur in women aged 40 to 74. More than 50% of cases of uterine cancer are reported in women over the age of 55, while only 1% of cases are found in women under the age of 40.
It can be said that ageing is one of the major risk factors for uterine cancer. Hence, women should be more vigilant for bleeding or discharge post-menopause. It can be a signal of uterine cancer.
Obesity
Women with obesity issues are two to four times more likely to develop uterine cancer than women of normal weight. Women who are very obese are 6 times more likely to develop uterine cancer than women of healthy weight.
This is mainly because the fat in the body can change other hormones into estrogen. And higher the level of estrogen hormones, greater the risk of developing uterine cancer. Obesity is also a well-known risk factor of diabetes which too increases the risk of uterine cancer.
Genetics
About 5 per cent of uterine cancer is linked to hereditary factors. Hereditary plays an important role in the development of cancer. However, a family history of cancer does not necessarily mean that one would get cancer.
Familial history of cancer or Lynch syndrome may result in a high risk of endometrial cancer. Women with these conditions are at 70% increased risk of developing endometrial cancer.
Tamoxifen
Tamoxifen is a drug that is used in the treatment or prevention of breast cancer. It reduces the effect of estrogen in breast tissues but amplifies the estrogen impact in the uterus. This increases the risk of uterine cancer, especially in post-menopausal women.
However, the risk of developing uterine cancer from tamoxifen is low, less than 1% per year. Also, the benefits of tamoxifen in preventing breast cancer outweighs the risk.
But still, it is important to discuss the risks before using tamoxifen for breast cancer treatment. Women who use Tamoxifen should be more attentive to any abnormal vaginal bleeding. Also, a yearly gynaecologic examination is advised!
Prolonged menstruation
This is a natural risk factor for uterine cancer. Women who had an early puberty (before the age of 12) and late menopause (after the age of 50) are at an increased risk of uterine Cancer.
The more the number of menstrual cycles, the greater is the risk. Women who have frequent menstrual cycles (less than 28 days) or have a history of polycystic ovarian syndrome (PCOS) have the same risk.
This is because of the increased exposure to estrogen hormones during their lifetime. The hormone estrogen plays a key role in the regulation of menstrual cycles. More menstruation cycles mean higher lifetime exposure to estrogen which is a known risk for uterine cancer.
No pregnancy
Researchers say that at least one pregnancy throughout the lifetime seems to reduce the risk of uterine cancer. This is because, during pregnancy, a woman’s body produces more progesterone and less estrogen.
Irregular mensuration cycles, infertility or no child by choice may cause an imbalance in estrogen and progesterone levels, which may increase the risk of uterine cancer.
Radiation therapy to the pelvic area
Radiation therapy to the pelvic area for the treatment of a different type of cancer can increase a woman’s risk of uterine cancer. Radiation may damage the healthy cells in the uterus, thus leading to cancer of the uterus.
History of retinoblastoma
Retinoblastomais a type of eye cancer, usually caused by an abnormal gene. It is a common cancer diagnosed in children. However, in some cases, retinoblastoma can occur in adults too. Researchers have found that a history of retinoblastoma may be linked to a higher risk of uterine sarcoma.
A history of other health issues like high blood sugar, high blood pressure, high levels of triglycerides, low levels of high-density lipoproteins in the blood or extra fat around the abdomen is also cited as a risk factor for uterine cancer.
All of these risk factors increase the risk of developing uterine cancer in a lifetime by some percentage. But none of these factors can guarantee the development of uterine cancer. There are many people who have been exposed to one or more of these risk factors, but have not reported of cancer.
Can Uterine Cancer Be Prevented?
Most cases of uterine cancer are caused by natural factors that are beyond one’s control. But there are a few lifestyle factors like obesity, diabetes etc. can further alleviate the risk. So, controlling these factors can lower the risk of uterine cancer to some extent.
Here are a few tips advised by experts to prevent uterine cancer:
- Taking birth control pills can reduce the risk of an overgrowth of the uterine lining.
- Using an UID (intrauterine device), a birth control device can lower the risk.
- Diabetic patients should take proper precautions to manage diabetes.
- All women should maintain balanced hormonal levels through healthy diet and exercise.
- Manage stress, depression, and sleep to control hormones.
- Getting early treatment for endometrial problems.
- Regular consultation and screening for endometrial problems or HNPCC cases.

What Are The Stages Of Uterine Cancer?
Staging of Uterine Cancer helps in proper diagnosis and planning for the treatment. It is staged in 4 levels ranging from stage I to IV, the severity increasing with each passed stage. The stages are discussed in details below:
- Stage 0 (Tis, N0, M0): Also known as carcinoma-in-situ, in this stage cancer cells are found only in the surface layer of cells of the endometrium.
- Stage I (T1, N0, M0): In this stage, cancer cells are found only in the uterus. It has not spread to lymph nodes or distant sites.
- Stage IA: In this earliest form of stage I Cancer and it lies in the endometrium only.
- Stage IB: Cancer has spread halfway or more into the myometrium but has not gone beyond the body of the uterus.
- Stage II (T2, N0, M0) Cancer cells are present in both the uterus and cervix but has not spread outside of the uterus.
- Stage III (T3, N0, M0) Cancer has spread beyond the uterus, but not beyond the pelvis.
- Stage IIIA – cancer has spread to the outer layer of the uterus or to the fallopian tubes, ovaries, and ligaments of the uterus.
- Stage IIIB – cancer has spread to the vagina or to the tissues around the uterus.
- Stage IIIC – cancer has spread to lymph nodes in the pelvis and/or around the aorta.
- Stage IV (T4, any N, M0) or (any T, any N, M1) Cancer has spread past the pelvic region and can affect the bladder, rectum, and more distant parts of the body.
- Stage IVA – cancer cells have spread to the inner lining of the rectum or urinary bladder.
- Stage IVB – cancer has spread to distant lymph nodes, the upper abdomen, the omentum, or to organs away from the uterus. It can be any size and may or may not have spread to lymph nodes.
- Stage IIIC – cancer has spread to lymph nodes in the pelvis and/or around the aorta.
Survival Rates Of Uterine Cancer?
Survival rate is a mere estimation calculated by taking into account the past records of uterine cancer patient’s survival. Usually, it is calculated for a period of 5 years. But these percentage should not be treated as a verdict. There are several factors that matter in determining the prognosis or survival rate of uterine cancer.
Here is the statistical data shared by researchers that can give a vague idea about the severity of the cancer at different stages:
| Stage | Survival Rate |
| 0 | 90% |
| IA | 88% |
| IB | 75% |
| II | 69% |
| IIIA | 58% |
| IIIB | 50% |
| IIIC | 47% |
| IVA | 17% |
| IVB | 15% |
Can Uterine Cancer Be Detected Early?
About 67% of uterine cancer cases are detected in an early stage. Because cancerous growth in the uterus often causes symptoms like vaginal bleeding, pelvic pain, vaginal discharge and discomfort.
Most cases of uterine cancer are diagnosed during a visit to the gynaecologist. In case the gynaecologist suspect cancer, he or she might suggest any of the following tests and screenings to confirm the presence of cancerous cells:
- Pelvic examination: If the symptoms of uterine cancer are reported then a gynaecologist may conduct a pelvic examination. In this process, the doctor observes the outer portion of the vulva by inserting two fingers of one hand while pressing the lower abdomen with the other hand. Sometimes, the doctor can also use a speculum to open up the vagina and look at the vagina and cervix for cancerous growths or tumor.
- Ultra sound: The doctor might recommend a simple ultrasound or a transvaginal ultrasound in case of uterine cancer suspicion. The simple ultrasound is done by moving a transducer over the skin of the lower part of the belly to capture images of the uterus, ovaries, and fallopian tubes. For a transvaginal ultrasound, the transducer is inserted into the vagina to check if the uterus contains a tumor, or if the endometrium is thicker than usual, or if there is a mass in the myometrium.
- Hysteroscopy: A lens on a special lighted telescope which is about 1/6 inch in diameter is called a hysteroscope. In this process, the hysteroscope is inserted into the vagina through the cervix, which allows the doctor to get a better view of the inner lining of the uterus. This allows the doctor to look for anything abnormal, cancerous cells or a polyp. Usually, patients are given local anaesthesia in this process.
- Biopsy: Biopsy is the most common and effective test for detecting uterine cancer. In biopsy, a very thin, flexible tube is inserted into the uterus through the cervix to extract a small amount of the cells from the uterus through suction. For a biopsy, the doctor might use local anaesthesia or prescribe anti-inflammatory drug like ibuprofen before the procedure.
- Dilatation & curettage: When enough information couldn’t be obtained by the above processes including biopsy then dilatation and curettage is used. In this procedure, the cervix is widened (dilated) so that a curette (a spoon-shaped instrument with a sharp edge) can be inserted into the uterus. This is done to remove cells, tissues or growths from the endometrium. It may be done with or without a hysteroscope.
What Are The Treatments Available For Uterine Cancer?
Uterine cancer in most cases are detected early and treated fairly. The treatment options for uterine cancer depend on multiple characteristics, like the stage, general health condition, root cause, age of the patient, their preference and many such factors. Weighing all the factors the oncologist could choose any of the following treatment options –
Depending on the stage and spread of the cancer cells, the doctor decides the extent of this surgery as –
- Simple hysterectomy: It accounts for about 8 out of 10 cases of Medullary Thyroid Cancer. It occurs mostly in older adults.
- Radical hysterectomy: In this the doctor removes the uterus, cervix and ovaries. The doctor may also remove all of the surrounding tissue and the upper part of the vagina. This is mostly done when cancer has spread to the cervix.
- Lymphadenectomy: In this process, the doctor removes the lymph nodes in the pelvis to determine if cancer has spread, and if additional treatment will be needed.
Radiation therapy is usually used as a treatment option at later stages of uterine cancer, mostly because of the possible side effects of radiation therapy. The doctor may also use radiation therapy combined with chemo or surgery as per the unique requirements of patients.
Radiation therapy includes
- External Radiation
- Internal radiation (brachytherapy)
Hormone therapy is used to:
- Increase the amount of progesterone
- Reduce the amount of estrogen
Chemotherapy too is used in cancer treatment at later stages, because of the toxicity. Doctors may advice chemotherapy before or after surgery, with or without radiation depending on what’s best for the patient.
Uterine cancer treatment also includes targeted therapy, immunotherapy and palliative care. Targeted therapy is the use of drugs that target specific cancer cells and kills them. Immunotherapy uses drugs that equips the patient’s natural defence mechanism to fight against cancer cells. Palliative care is specialized medical care that focuses on providing relief while undergoing aggressive treatments like surgery, chemotherapy or radiation therapy.
There are several cancer treatment options available today for uterine cancer. The healthcare providers devise the best care plan unique for each patient.

Uterine Cancer, if detected at early stages is easy to cure. Endometrial Cancer is usually cured with proper treatment while uterine sarcoma is harder to cure. Removing the uterus along with the surrounding affected organs is generally the go to solution, though it ends up in menopause and infertility.
Though cure at later stages become slim, but there is a great possibility of finding cure even after cancer has metastasized. The patient and healthcare team should work closely towards the progress of treatment.
Open conversations about the symptoms, side-effects, mental health, emotional conditions, coping and recovering helps in better prognosis.
03

People who have ticked on one or more of the risk factors should go for regular screenings and tests. Post-menopausal women, obese women, women with hormonal issues, women with frequent periods, women using tamoxifen or exposed to any other risks should consult a gynaecologist regularly with or without symptoms.
Women who in doubt for any of the symptoms should consult a gynecologist and get their doubts cleared. Even a faint or ignorable symptom could still be an early signal, which when attended could save a lot of damage.
02

Uterine Cancer is among those few cancer types that are usually detected early for the prominent symptoms it produces. Abnormal vaginal bleeding, vaginal discharge, pelvic pain, a tumorous mass, bloating often lead the patient to the doctor’s clinic resulting in diagnosis.
